Type 1 vs Type 2 vs Gestational Diabetes: Key Differences Explained
Barbara Davis Center Faculty • November 2, 2022
TL;DR
Type 1, type 2, and gestational diabetes are completely different conditions with distinct causes, treatments, and outcomes. Type 1 is an autoimmune disease requiring lifelong insulin, type 2 is often linked to lifestyle and can sometimes be prevented or reversed, and gestational diabetes occurs during pregnancy and may increase future risk of Type 2. Understanding these differences is essential for proper management and awareness.
What Is Type 1 Diabetes?
It’s important to know that type 1, type 2 and gestational diabetes are different diseases. While they all deal with insulin and the body, their causes and treatments are very different. Type 1 diabetics cannot make their own insulin. Type 1 is a genetic, auto-immune disease. It is thought that type 1 is present in the body’s genetic code and then it presents at various times. Basically meaning, it’s lying there in wait and decides to show itself at various ages.
Most type 1 patients get diagnosed in their childhood and when they are adolescents, however it can happen later in life as an adult. The body begins attacking its own pancreatic cells, specifically the islet cells that make insulin in our bodies. It attacks these cells so aggressively that the patient stops being able to make any insulin whatsoever.
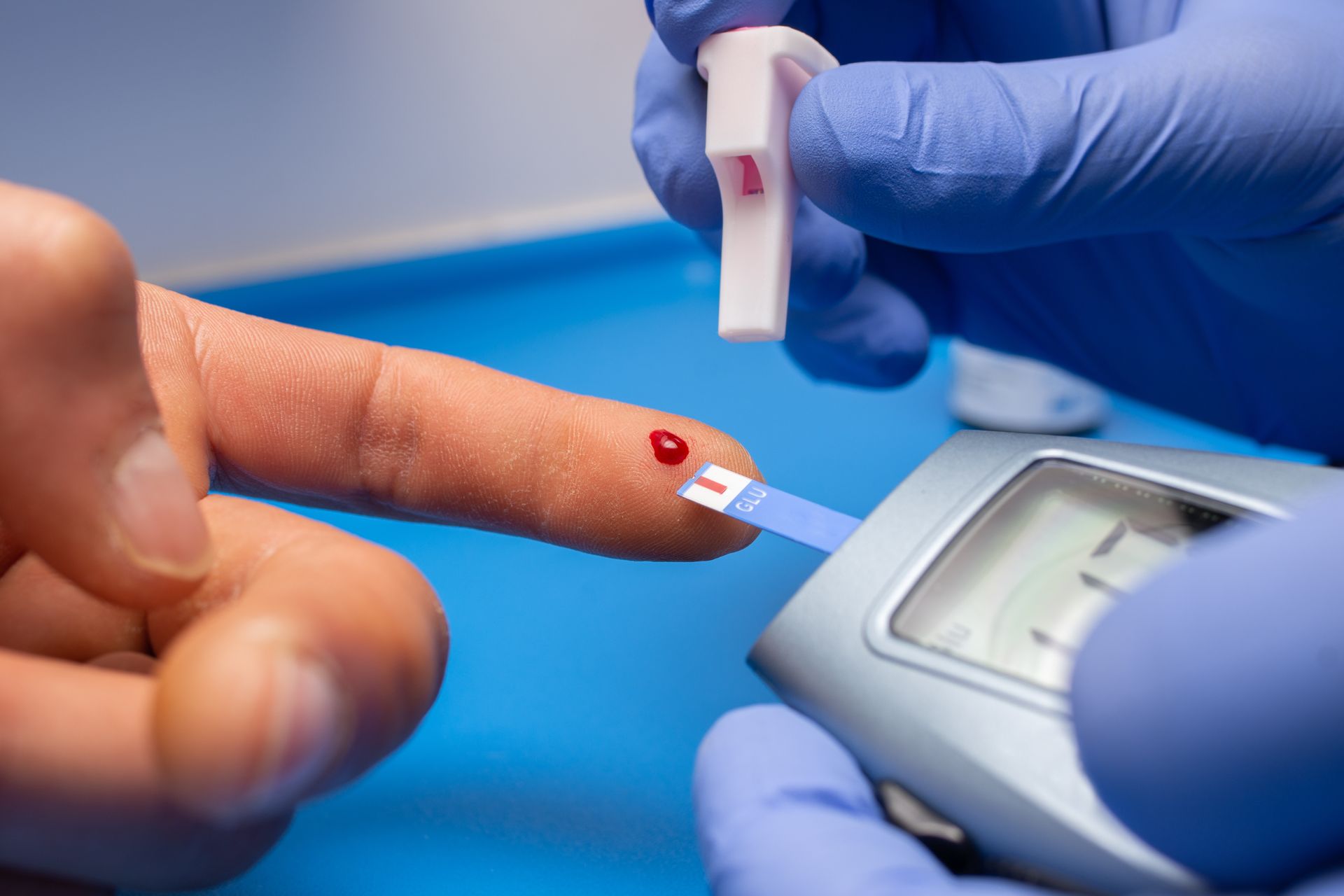
Insulin processes the carbohydrates we eat and feeds our cells. If we don’t feed our cells, we have too much sugar in our system which wreaks havoc on everything from your kidneys to your eyes to the mood you are in. You cannot live (for long) without insulin.
Only 100 years ago, a person diagnosed with type 1 diabetes would be lucky to stay alive for two more years and that life would be one of misery and starvation. This auto-immune attack on the pancreas cannot be prevented. If it’s in the genetic cards for you, you can’t stop it. Type 1 cannot be caused by an unhealthy diet, eating too much sugar, obesity or lifestyle issues. It cannot be cured (yet!) and patients will live with the disease for the rest of their lives.
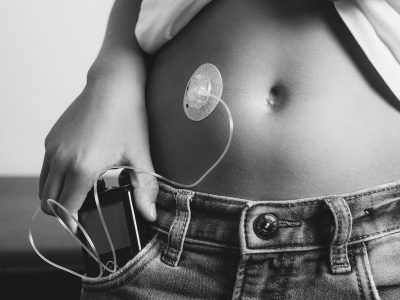
Thankfully, we now have treatments and technology to manage type 1 diabetes but that is what it is – a lifelong management. Patients take synthetic insulin via injections or by using an insulin pump and do all the work and insulin calculations a normal pancreas does naturally in the body. They also constantly monitor their blood sugar numbers, trying to stay within a normal range. When we say we manage it, we mean it is top of mind every minute of every day. Tons of different things affect blood sugar. Food is the biggest one, but blood sugar is also affected by exercise, illness, sleep, co-occurring conditions, menstruation, stress, medication, altitude, weather… and the list goes on.
Managing all these things and injecting insulin for various situations is a full time, exhausting job. And even the type 1 patients who have a lifetime of good control will feel the effects of the disease on their body and through various complications. Only 5% of the total diabetes population has type 1 diabetes, although the number of newly diagnosed type 1 patients is increasing each year.
What Is Type 2 Diabetes?
Type 2 diabetics CAN make their own insulin, but they either aren’t making enough or insulin is not working properly in the body. Type 2 can be caused by an unhealthy diet and obesity; however, there is also a correlation between type 2 diabetes and hereditary genetics. Similar to cholesterol – if your grandpa has high cholesterol and your dad has high cholesterol, you are likely headed for the same outcome. Same with type 2 diabetes, there is a heredity genetic component of it.
Type 2 diabetes can be prevented, even in someone with a family history of it, and it may also be reversed. Managing diet, maintaining activity/exercise, and monitoring blood sugar levels allow the body to process insulin efficiently and make enough of it.
Some type 2 patients take oral medication to assist their body with the insulin they are making. These medications help by delaying the breakdown of carbohydrates and reducing glucose absorption. Type 2 diabetics may also manage their diabetes by taking synthetic insulin via injections.
Like type 1 diabetics, type 2 diabetes may be affected by stress, illness, sleep, and may experience complications and even death from uncontrolled type 2 diabetes. 95% of diabetics have type 2 diabetes.

What Is Gestational Diabetes?
And finally, there is gestational diabetes, which affects some pregnant women. During pregnancy, your body makes more hormones and goes through other changes, such as weight gain. These changes cause your body’s cells to use insulin less effectively.
Gestational diabetes typically does not present symptoms, so patients need to be tested. Treatment includes monitoring blood sugar levels, engaging in physical activity and eating the right foods at the right times. For most patients, gestational diabetes goes away soon after the delivery, but it can be a pre-curser to type 2 diabetes later in life. Every year in the United States, 2-10% of pregnancies will be affected by gestational diabetes.