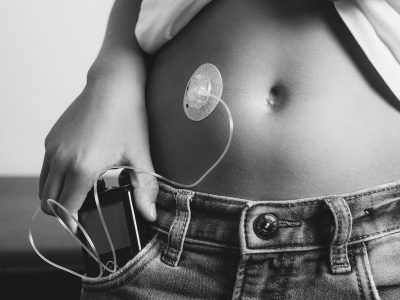
Meet the Colorado doctor helping Hispanic families with Type 1 diabetes
Graham Daugherty • July 25, 2016
By Joanne Davidso
First published by The Denver Post. See the original article by clicking here.
The roads that led Dr. Andrea Gerard-Gonzalez to the Barbara Davis Center for Diabetes on the Anschutz Medical Campus in Aurora weren’t all eight-lane expressways.
A few of them weren’t even covered in asphalt.
But each can be seen as a metaphor in the journey that brought her to Colorado, where she is making an important difference in the health of youngsters of Latin descent who are Type 1 diabetics.
As director of the Barbara Davis Center’s Hispanic/Latino Diabetes Care Team, Gerard-Gonzalez continues to develop and expand culturally appropriate ways to not only improve the delivery of diabetes care for the 800 youngsters with whom her team works, but to educate family members about the disease, eliminate stigmas and build a sense of community.

Ultimately, the 36-year-old endocrinologist hopes to see medical facilities in other cities adopt the model on which her program is based; she is also working to modify it for other ethnic cultures.
“In the United States, Hispanic children under-utilize diabetes care technology and have higher HbA1c levels than non-Hispanic white children,” explains Dr. Marian Rewers, the Barbara Davis Center’s executive director. “This is likely related to language barriers, cultural barriers and the limited availability of Spanish-speaking staff and resources.”nn(HbA1c, or glycated hemoglobin levels, are determined through a blood test that gives doctors an overall picture of a patient’s average blood-sugar levels over a period of weeks or months).
“It’s painful for me to see such a disparity in outcomes,” Gerard-Gonzalez says. “Just translating printed materials isn’t enough. You have to work with the people in ways in which they are comfortable.”
After graduating first in her class from the prestigious Universidad La Salle School of Medicine in her native Mexico City, Gerard-Gonzalez set out for Chiapas, one of Mexico’s southernmost states, to complete a two-year internship at a tiny clinic ill-equipped to meet anything other than the most basic medical needs.
It was located in what she says was an “incredibly beautiful area … out in the middle of nowhere.” The nearest hospital was two hours away, reached by negotiating a bumpy, dusty — or muddy — unpaved road where farm animals roamed freely.
Little did she know how well the geographic and cultural challenges she faced would prepare her for her current job.
“You arrive filled with joy and expectations about how you’re going to change things for the better, help nourish the society. But then you find that you don’t understand their language or culture — it was a mostly indigenous population and not everyone spoke Spanish — and that they don’t want you and don’t trust you.”
Establishing trust and respect was difficult, she admits in an interview conducted during her lunch break in a conference room at the Barbara Davis Center.
She gained it after two touch-and-go medical emergencies — one in which she saved the life of both mother and baby during a complicated delivery, and the other involving a child who arrived at her clinic near death because of untreated diabetes. She was able to convince the child’s parents that he needed insulin to survive and that hospitals shouldn’t be seen as scary places.
“One of the greatest things that I learned in Chiapas is that there are many right ways to do things, not just the one way you think is right. (That experience) taught me that we need to work with the culture of the communities we serve and make things appropriate for them.”
Which is exactly what she is doing at the Barbara Davis Center.
The “unique and innovative model” that she and her team developed includes family-style shared medical appointments, educational materials written in Spanish and activities that are culturally sensitive and appropriate. The goal is to reduce costs associated with treating high-risk patients and build a strong sense of community within Colorado Latino patients with Type 1 diabetes.
“We alternate one-on-one visits with 45-minute sessions where Spanish-speaking professionals talk about things like carb counting, healthy eating and the importance of exercise.”
At first, she said, “We thought 45 minutes would be too much time because Latin families — and we have patients not just from Mexico but from Puerto Rico, Cuba and Guatemala — tend to be very private about their personal stuff. They might not know what diabetes is, and so a parent can feel guilty because their child has it. Which is what we want to eliminate.”
To her surprise and delight, “The conversation never stopped, even when the 45 minutes were up. They’d leave the building, but we’d see them continuing to chat on the sidewalk and in the parking lot.”
When her internship in Chiapas ended, Gerard-Gonzalez and her husband, Alejandro Ayestarán, a civil engineer, made the difficult decision to leave Mexico and move to Miami, where she joined the pediatrics staff at Miami Children’s Hospital.
“It was very hard to leave our loved ones behind,” she admits, “but my husband wanted to get an MBA and I had this great opportunity to get further training at one of the top children’s hospitals in the U.S.”
From Miami, the couple moved with their dog, Emma, to California, where she completed a fellowship in endocrinology at the University of California San Francisco. Three years ago, she gave birth to twins Sofia and Alex.
At the conclusion of her fellowship she was recruited by the Barbara Davis Center and the family moved to Colorado.
It’s a move she does not regret.
“I would have been a good doctor in Mexico but I might not have been able to make the impact I wanted to have. The Latin people are proud people and they don’t want to be judged, so we have to make them feel strong, to better understand diabetes and eliminate any guilt they may feel because their child has diabetes. We are able to do that here at the Barbara Davis Center.”
—
Joanne Davidson was The Denver Post’s society editor for 29 years before retiring in July, 2015. She quickly discovered she wasn’t ready for the rocking chair, so she dusted off her evening gowns and returned to the paper as a freelance reporter, writing feature stories and covering charitable fundraising events in the metro area. When she’s not attending a gala, you can find her out walking her dogs or sampling the food in one of Denver’s great restaurants.